Development status
Solid cancer: Therapeutic for Non-Small Cell Lung Cancer
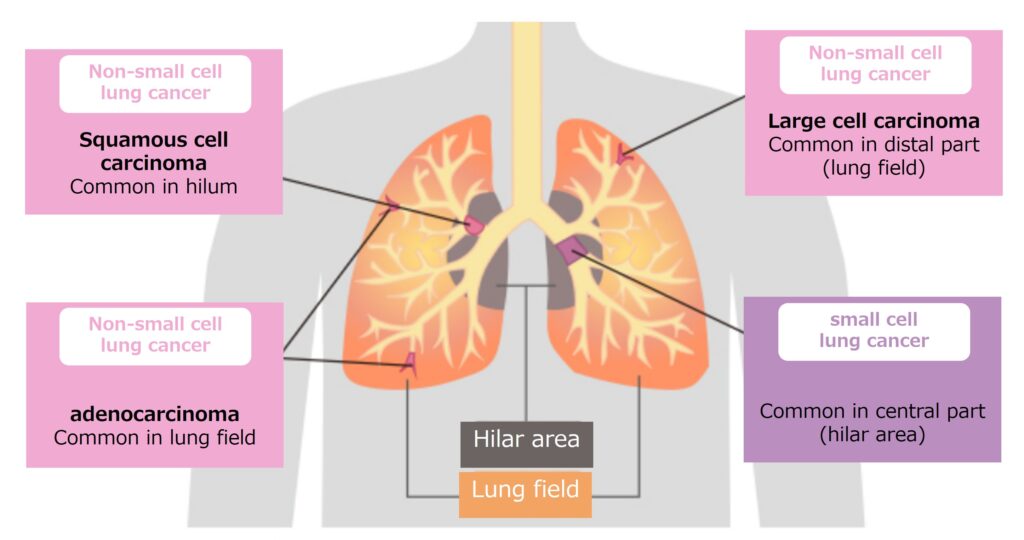
Lung cancer is the leading cause of cancer death with a poor prognosis. In Japan, the number of people newly diagnosed with lung cancer has been increasing every year: in 2019, the number of lung cancer cases was 84,325 in men and 42,221 in women, and in 2020, the number of deaths was 53,247 in men (1st cause in men) and 22,338 in women (2nd cause in women). Lung cancer is frequently classified by histological type into “small cell carcinoma,” “adenocarcinoma,” “squamous cell carcinoma,” and “large cell carcinoma,” and all but small cell carcinoma are classified as non-small cell lung cancer. Non-small cell lung cancer accounts for 80-85% of all lung cancers.
Current Treatments and Challenges
Treatment for non-small cell lung cancer can be broadly categorized into surgery, drug therapy, and radiation therapy, and a combination of these is used. The treatment depends on the stage of the disease. Surgery is mainly performed in stages 1, 2, and part of stage 3, while stage 4 is mainly drug treatment, since the cancer is metastasized to other organs.
Currently, platinum-based chemotherapy and immune checkpoint inhibitors are used as first-line treatment for advanced non-small cell lung cancer without mutations in the driver genes (genes that play a direct role in cancer development and progression), but only small number of cases can be cured. Chemotherapy with docetaxel and other anticancer agents is used as second-line treatment, but the stable condition without cancer progression lasts only 3 months, and therefore third-line treatment is required. Though the combination of immune checkpoint inhibitors, anti-PD-1 antibody nivolumab and anti-CTLA-4 antibody ipilimumab is the treatment option, the combination has the problems that immune-related side effects increase and that two antibodies cause high medical costs. A multicenter clinical trial in untreated advanced or recurrent non-small cell lung cancer (JCOG 2007 study, the specified clinical research) showed approximately 7.4% (11 out of 148 patients) deaths beyond the expected range, in which a causal relationship to treatment could not be ruled out, and the study was discontinued on March 30, 2023. These are the same problems that arise in the treatment of advanced non-small cell lung cancer, and drugs that improve the efficacy of anti-PD-1 antibody as third-line therapy in advanced non-small cell lung cancer are long awaited.
Characteristics of Our Solution
In research and development for malignant melanoma, we discovered that RS5614 is an immune checkpoint inhibitor and that its efficacy is further enhanced when combined with nivolumab, and a Phase II investigator-initiated clinical trial confirmed that the combination of nivolumab and RS5614 is effective in the patients refractory to nivolumab. The findings are applied to the study for non-small cell lung cancer. In a preclinical study conducted in a mouse model of non-small cell lung cancer in collaboration with Hiroshima University, we confirmed that, as in the malignant melanoma model, the combination administration of an anti-PD-1 antibody and RS5614 showed a higher anti-tumor effect than the administration of an anti-PD-1 antibody alone.
The efficacy of RS5614 is also expected since PAI-1 is involved in tumor progression of lung cancer, as well as in the enhancement of proliferative potential and angiogenesis of cancer cells, and that lung cancer cells that become resistant to nivolumab express high levels of PAI-1, based on research conducted at Hiroshima University.
RS5614 is a drug with a high safety profile and is inexpensive because it is chemically synthesized. The combination of nivolumab and RS5614 may be more useful than the combination of nivolumab and ipilimumab, which causes many serious side effects.
Based on the inhibitory activity of the PAI-1 inhibitor RS5614 on immune checkpoint molecules, we have been conducting this study in collaboration with Hiroshima University, etc. The Phase II investigator-initiated clinical trial is conducted to evaluate the efficacy and safety of RS5614 in combination with nivolumab in patients with unresectable advanced or recurrent non-small cell lung cancer who have received at least two prior chemotherapies (third-line treatment).
In October 2022, Renascience entered into a collaboration agreement with Hiroshima University for non-clinical and clinical studies for non-small cell lung cancer. In April 2023, Renascience further concluded an agreement on comprehensive research collaboration with Hiroshima University to establish a center for open innovation (Hiroshima University x Renascience Open Innovation: HiREx), since the phase of the collaborations has progressed from non-clinical to the clinical stage (an investigator-initiated clinical trial). By taking the advantage of the features and strengths of Hiroshima University, we plan to conduct multiple joint research and development of pharmaceuticals and various software as a medical device, including implementation of investigator-initiated clinical trials, and establish an open innovation center for the purpose of improving and promoting R&D efficiency and human resource development. This clinical study for non-small cell lung cancer is led primarily by HiREx.